Вирус папилломы человека высокого канцерогенного риска (ВПЧ ВКР) является этиологической причиной рака шейки матки, а также может привести к развитию предракового состояния – анальной интраэпителиальной неоплазии (АИН), что сопровождается высоким риском развития рака анального канала [1, 2].
ВИЧ-инфекция увеличивает риск персистенции ВПЧ ВКР, тем самым ухудшая прогноз и способствуя развитию онкологического процесса, поэтому среди ВИЧ-инфицированных пациентов заболеваемость ВПЧ-ассоциированным раком ануса регистрируется значительно чаще [3–5].
Другие факторы риска, связанные с анальной дисплазией, включают снижение количества CD4+-лимфоцитов [6] и курение никотиносодержащей продукции [7, 8]. Некоторые исследователи предполагают, что восстановление иммунитета с помощью антиретровирусной терапии (АРТ) у больных ВИЧ-инфекцией снижает, но не устраняет риск рака ануса [9, 10].
Данные мультицентрового исследования показали, что в популяции ВИЧ-инфицированных женщин в 27% случаях диагностируется высокая степень плоскоклеточного интраэпителиального поражения в анусе [11]. Поэтому таким женщинам рекомендуется проводить скрининг на ВПЧ-ассоциированные заболевания ануса, независимо от результатов цервикального исследования [12]. При этом ряд исследователей рекомендуют проводить скрининг предраковых заболеваний ануса всем женщинам с ВИЧ-позитивным статусом в возрасте от 35 лет и старше [11, 13].
На фоне значительного снижения частоты ряда оппортунистических инфекций возрастает роль онкологической патологии, в том числе рака ануса, способных повлиять на долгосрочное течение ВИЧ-инфекции у женщин. Рак ануса может стать новой клинической проблемой у ВИЧ-инфицированных женщин, особенно в условиях ограниченных ресурсов (отсутствия единого подхода и четких национальных стандартов проведения скрининга, отсутствия расходных материалов и достаточного количества отечественных диагностических наборов реагентов для его осуществления). Все вышеперечисленное представляет серьезную проблему не только для клинической медицины, но имеет важное социально-экономическое значение, так как затрагивает трудоспособное население.
Цель исследования – изучение распространенности ВПЧ ВКР при одновременном исследовании биологического материала из цервикального канала и ануса у ВИЧ-инфицированных женщин.
Материалы и методы
Работа проводилась в период с августа 2018 г. по июль 2019 г. на базе Центрального НИИ эпидемиологии Роспотребнадзора (далее – ЦНИИЭ). В исследовании приняла участие 101 женщина с ВИЧ-положительным статусом, проживающая в Москве и Московской области. Критериями включения служили женский пол от рождения, возраст старше 18 лет, подписанное информированное согласие на участие в исследовании; критерием исключения – отсутствие возможности понять смысл информированного согласия.
Подтверждение ВИЧ-статуса в исследовании осуществляли на основании данных медицинской документации, содержащей положительные результаты лабораторного тестирования (реакции иммунного блота).
У всех участниц определяли количество CD4+-лимфоцитов и уровень РНК ВИЧ.
От каждой участницы исследования для последующего ПЦР-тестирования получен биологический материал из цервикального канала и ануса. Взятие соскоба эпителиальных клеток цервикального и анального каналов в транспортную среду для жидкостной цитологии BD SurePath (BD Diagnostics, США) проводили с помощью эндоцервикальной щетки – урогенитального зонда типа F (Changzhou Chuangjia Medical Applience Co, КНР).
Во всех образцах биологического материала определяли ДНК ВПЧ ВКР методом полимеразной цепной реакции с детекцией флуоресцентного сигнала в режиме реального времени (ПЦР-РВ). ВПЧ-тестирование позволило выявить генотипы ВПЧ ВКР (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, 68) и определить границы биологической значимости при анализе получаемых результатов. При выполнении тестов контролировали качество взятия биологического материала в образце. При недостаточном количестве эпителиальных клеток (< 500) в исследуемом биологическом материале образец признавали невалидным.
Экстракцию ДНК ВПЧ проводили с помощью комплекта реагентов «АмплиСенс® ДНК-сорб-Д» (№ РЗН 315/3503, ЦНИИЭ). Выявление и типирование ДНК ВПЧ ВКР выполняли с использованием комплекса реагентов «АмплиСенс® ВПЧ ВКР скрин-титр-14-FL» (№ РНЗ 2017/5387) и «АмплиСенс® ВПЧ ВКР генотип-титр-FL» (№ РНЗ 2017/6533) того же производителя.
Для постановки и анализа результатов амплификации использовали прибор с системой детекции флуоресцентного сигнала в режиме реального времени Rotor-Gene Q (QIAGEN, Германия) в соответствии с инструкциями производителя.
Статистические данные обрабатывали с использованием программного пакета Microsoft Excel (Windows XP) и SPSS16 (допустимая ошибка Е = 5%). Были использованы показатели описательной статистики: средняя (М), медиана (Ме), стандартное отклонение (m), минимум (min), максимум (max), 95% ДИ. Для сравнения количественного показателя применяли критерий Стьюдента. При анализе различий между группами по качественным признакам использовали критерий χ2. Различия между группами считали статистически значимыми при р < 0,05.
Результаты и обсуждение
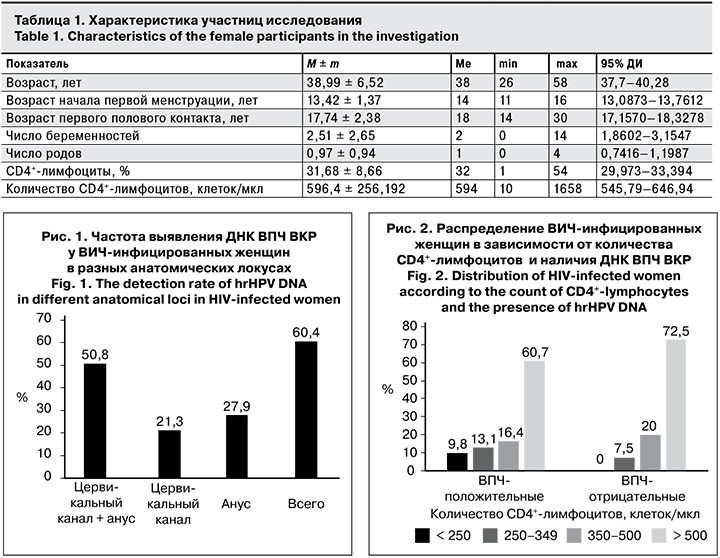
В ходе исследования обследована 101 ВИЧ-инфицированная женщина. Подробная характеристика участниц представлена в табл. 1.
Среди участниц исследования преобладали женщины в возрасте 38,99 ± 6,52 года [Ме – 38 лет (min – 26, max – 58)], из них 6 (5,9%) были моложе 30 лет.
67 (66,3%) женщин заразилась ВИЧ-инфекцией половым путем, 27 (26,7%) – при использовании внутривенных психоактивных веществ. Сопутствующие заболевания имели 36 (35,6%) женщин, ранее не проводили скрининг предраковых заболеваний шейки матки 27 (26,7%).
Имели опыт, но прекратили курение никотиносодержащих изделий на момент проведения исследования 48 (47,5%) участниц; 30 (29,7%) продолжали курить; 21 (20,8%) отметила, что никогда не курила; 2 (2%) имели однократный опыт курения.
Среди участниц исследования преобладали женщины с количеством CD4+-лимфоцитов 596,4 ± 256,192 клеток/мкл, < 250 клеток/мкл имели 6 (5,9%) пациенток, > 500 клеток/мкл – 66 (65,3%). АРТ получали 95 (94,1%) женщин, при этом у 94 (98,9%) из них РНК ВИЧ была ниже определяемого уровня. Лишь у 1 пациентки зарегистрировали РНК ВИЧ выше уровня детекции на фоне АРТ, и это было связано с недавним ее началом.
В результате проведения ВПЧ-теста у 61 (60,4%) женщины выявлена ДНК ВПЧ ВКР (рис. 1), при этом частота выявления ДНК ВПЧ ВКР одновременно в цервикальном канале и анусе составила 50,8%. Обращает на себя внимание тот факт, что изолированно ДНК ВПЧ ВКР выявлена в анусе в 27,9% случаев, в цервикальном канале – в 21,3%. Учитывая положительный результат ВПЧ-тестирования одновременно в 2 обследованных локусах, а также изолированно в анусе, общая частота выявления ДНК ВПЧ ВКР в анусе составляла 78,7%.
Установлено, что среди ВИЧ-инфицированных пациенток с положительным результатом ВПЧ-теста преобладали женщины молодого возраста – 39,2 ± 6,998 года (min – 26, max – 58). В группе ВИЧ-инфицированных с отрицательным результатом теста также преобладали женщины молодого возраста, но средний возраст был немного выше и составил 38,65 ± 5,78 года (min – 27, max– 54).
Распределение по возрасту женщин с положительным и отрицательным результатом ВПЧ-теста не выявило статистически значимых различий (t-критерий Стьюдента = 0,39; p = 0,695293; f = 99; критическое значение t-критерия = 1,987 при уровне значимости α = 0,05). Учитывая полученные данные, необходимо рекомендовать скрининг в виде ВПЧ-теста всем ВИЧ-инфицированным женщинам, имеющим фактор риска, вне зависимости от возраста.
Среди никогда не куривших пациенток ВПЧ ВКР выявлен в у 12 (57%), в то время как в группе имеющих опыт курения – у 49 (62,8%) (χ2 = 0,543; p = 0,462). Но при более подробном изучении влияния курения на частоту выявления ВПЧ ВКР значимых отличий не обнаружено.
Количество СD4+-лимфоцитов у женщин с положительным результатом ВПЧ-теста составило 568,57 ± 284,54 клеток/мкл (min –10, max – 1658), в то время как у женщин с отрицательным результатом – 638,75 ± 201,7 клеток/мкл (min – 255, max – 999). Распределение всех женщин по данному показателю не выявило статистически значимых различий (t-критерий Стьюдента = 1,45; p = 0.150386; f = 99; критическое значение t-критерия = 1,987 при уровне значимости α = 0,05). Но при более подробном изучении установлено, что количество СD4+-лимфоцитов < 250 клеток/ мкл у ВПЧ-отрицательных пациенток не зарегистрировано, а в группе ВПЧ-положительных этот показатель достигал 9,8% (χ2 = 4,183; p = 0,041) (рис. 2). У ВИЧ-инфицированных женщин с отрицательным или положительным ВПЧ-тестом при количестве СD4+-лимфоцитов > 500 клеток/мкл значимых отличий выявлено не было (χ2 = 1,497; p = 0,222).
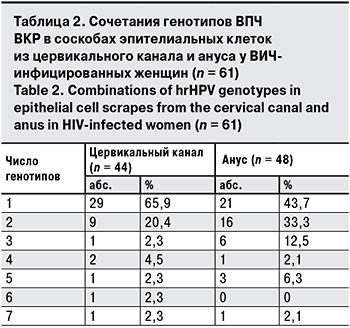 Учитывая полученные данные, мы можем сделать вывод, что у женщин с низким количеством СD4+-лимфоцитов ДНК ВПЧ ВКР выявляется чаще, и это требует назначения таким пациенткам дополнительных исследований для диагностики и профилактики злокачественных поражений шейки матки и ануса. Полученные результаты подтверждают, что пациенты с ВИЧ-инфекцией являются группой риска по развитию онкопатологии, обусловленной ВПЧ ВКР [6, 9, 10, 12, 14].
Учитывая полученные данные, мы можем сделать вывод, что у женщин с низким количеством СD4+-лимфоцитов ДНК ВПЧ ВКР выявляется чаще, и это требует назначения таким пациенткам дополнительных исследований для диагностики и профилактики злокачественных поражений шейки матки и ануса. Полученные результаты подтверждают, что пациенты с ВИЧ-инфекцией являются группой риска по развитию онкопатологии, обусловленной ВПЧ ВКР [6, 9, 10, 12, 14].
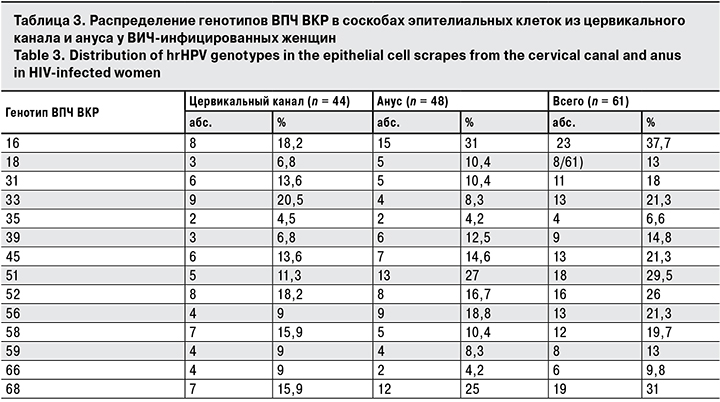
У ВИЧ-инфицированных женщин в цервикальном канале 1 генотип ВПЧ ВКР выявляли в 65,9% случаев, в анальном канале – лишь в 43,7%, При этом в образцах соскобов эпителиальных клеток из ануса обнаруживали одновременно от 1 до 7 генотипов ВПЧ ВКР (табл. 2).
В целом у обследованных женщин были обнаружены все 14 генотипов ВПЧ ВКР. Определение генотипа ВПЧ ВКР в исследованных образцах показало высокую распространенность ВПЧ 16 и 68 генотипов (37,7 и 31% соответственно), реже всего встречались 35 и 66 генотипы (6,6 и 9,8% соответственно), а 18 генотип уступал лидерство генотипам 16 и 68 (табл. 3).
Распространенность генотипов ВПЧ ВКР у ВИЧ-инфицированных женщин заметно различается в зависимости от исследуемого локуса (см. табл. 3). В соскобе из цервикального канала лидировали генотипы 16, 33 и 52 (18,2, 20,5 и 18,2% соответственно), в то время как в соскобах из ануса – генотипы 16 и 51 (31 и 27% соответственно).
У 21 (67,7%) из 31 ВИЧ-инфицированной женщины при одновременном обследовании 2 изучаемых локусов в соскобе эпителиальных клеток из ануса зафиксированы генотипы ВПЧ ВКР, отсутствующие у них в соскобе изцервикального канала. При этом в соскобе из ануса у 12 (38,7%) пациенток число выявленных генотипов ВПЧ ВКР было больше, чем в цервикальном канале.
Полученные данные свидетельствуют о необходимости выявления всех 14 генотипов ВПЧ ВКР в цервикальном канале и анусе у женщин с ВИЧ-позитивным статусом.
Обсуждение
У ВИЧ-инфицированных женщин во всем мире отмечают высокую частоту выявления аногенитальной папилломавирусной инфекции и повышенный риск развития онкологической патологии по сравнению с общей популяцией [2, 3, 15, 16].
ВПЧ ВКР, являющийся причиной рака шейки матки и рака ануса, широко распространен у ВИЧ-инфицированных женщин в Московском регионе: по результатам ВПЧ-тестирования образцов соскоба эпителиальных клеток ануса и цервикального канала, он составляет 60,4%. 27,9% случаев выявления ДНК ВПЧ ВКР приходится на изолированную локализацию в анусе, что создает риски для развития предраковых заболеваний шейки матки в случае, если женщина практикует аногенитальные контакты и не осведомлена о путях передачи и мерах профилактики папилломавирусной инфекции.
Инфицирование несколькими типами ВПЧ среди женщин с ВИЧ-позитивным статусом встречается чаще, чем в общей популяции, и чаще приводит к риску развития онкопатологии [16–18]. Результаты проведенного исследования показали высокую частоту выявления в эпителиальных клетках ануса ДНК сразу нескольких типов ВПЧ ВКР (56,3%), что в отсутствие диагностики аногенитальных ВПЧ-ассоциированных заболеваний несет угрозу здоровью трудоспособного женского населения. Поэтому становятся особенно актуальными рекомендации ряда исследователей о необходимости проведения скрининга на ВПЧ-ассоциированные заболевания ануса у ВИЧ-инфицированных женщин, независимо от результатов цервикального обследования [11–13].
Несмотря на то что ВИЧ-инфицированные женщины подвержены высокому риску рака ануса, опубликовано недостаточно данных о распространенности, естественном течении ВПЧ-ассоциированных заболеваний ануса, а также о потенциальных стратегиях скрининга предраковых изменений указанной локализации в этой группе риска [2]. Безусловно, роль различных типов ВПЧ ВКР в развитии ВПЧ-ассоциированных предраковых заболеваний и онкологической патологии ануса еще предстоит подробно изучить.
Возможно, инфраструктура для скрининга предраковых заболеваний шейки матки и рака шейки матки, основанная на ВПЧ-тестировании с выявлением 14 генотипов ВПЧ ВКР, может быть использована в качестве основы для разработки алгоритма скрининга предраковых изменений ануса у всех ВИЧ-инфицированных женщин.
Выводы
1. Распространенность аногенитальной папилломавирусной инфекции у ВИЧ-инфицированных женщин в Московском регионе по результатам тестирования образцов из цервикального канала и ануса составила 60,4%.
2. Показана высокая распространенность ВПЧ ВКР у ВИЧ-инфицированных женщин по результатам ВПЧ-тестирования образцов соскоба эпителиальных клеток цервикального канала (72,1%) и ануса (78,7%).
3. В 27,9% случаях у ВИЧ-инфицированных женщин наблюдалось изолированное поражение ануса, что позволяет рекомендовать скрининг ВПЧ-ассоциированных заболеваний ануса в отсутствие патологии шейки матки.
4. При одновременном выявлении ВПЧ ВКР в соскобе эпителиальных клеток из цервикального канала и ануса в 67,7% случаев наблюдалось несоответствие зарегистрированных генотипов ВПЧ ВКР.
5. Соотношение выявляемых генотипов ВПЧ ВКР у ВИЧ-инфицированных женщин значительно различается в зависимости от исследуемого локуса.
6. Наибольшая частота одновременного выявления нескольких (от 2 до 7) генотипов ВПЧ ВКР выявлена в образцах соскоба эпителиальных клеток ануса и составляет 56,3%.
7. Полученные результаты подчеркивают необходимость проведения скрининга предраковых заболеваний шейки матки и ануса, основанного на ВПЧ-тестировании с выявлением 14 генотипов ВПЧ ВКР у всех ВИЧ-инфицированных женщин.
8. Требуется разработка алгоритмов диагностики ВПЧ-ассоциированных заболеваний ануса (регистрация расходных материалов для взятия образцов соскоба эпителиальных клеток ануса и разработка диагностических наборов реагентов).
9. Необходимо проводить дополнительное консультирование ВИЧ-инфицированных женщин о необходимости проведения скрининга ВПЧ- ассоциированных заболеваний как шейки матки, так и ануса.



